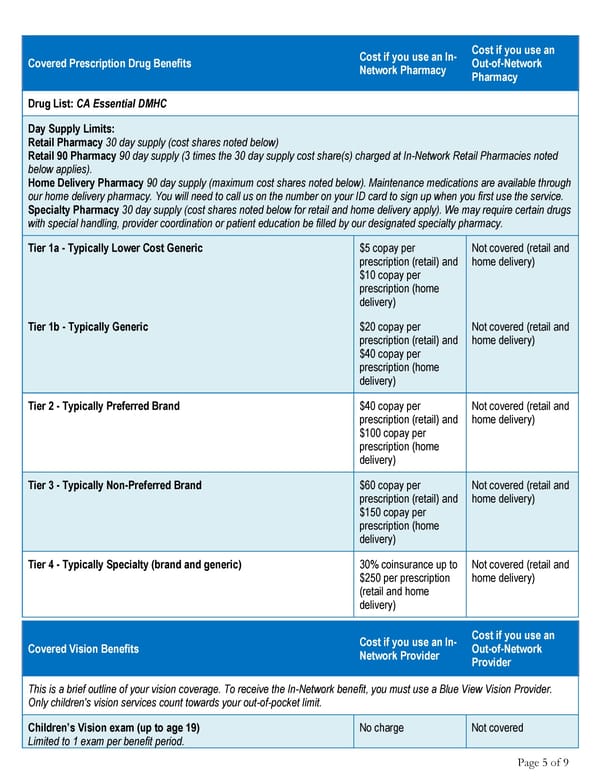
Cost if you use an In- Cost if you use an Covered Prescription Drug Benefits Network Pharmacy Out-of-Network Pharmacy Drug List: CA Essential DMHC Day Supply Limits: Retail Pharmacy 30 day supply (cost shares noted below) Retail 90 Pharmacy 90 day supply (3 times the 30 day supply cost share(s) charged at In-Network Retail Pharmacies noted below applies). Home Delivery Pharmacy 90 day supply (maximum cost shares noted below). Maintenance medications are available through our home delivery pharmacy. You will need to call us on the number on your ID card to sign up when you first use the service. Specialty Pharmacy 30 day supply (cost shares noted below for retail and home delivery apply). We may require certain drugs with special handling, provider coordination or patient education be filled by our designated specialty pharmacy. Tier 1a - Typically Lower Cost Generic $5 copay per Not covered (retail and prescription (retail) and home delivery) $10 copay per prescription (home delivery) Tier 1b - Typically Generic $20 copay per Not covered (retail and prescription (retail) and home delivery) $40 copay per prescription (home delivery) Tier 2 - Typically Preferred Brand $40 copay per Not covered (retail and prescription (retail) and home delivery) $100 copay per prescription (home delivery) Tier 3 - Typically Non-Preferred Brand $60 copay per Not covered (retail and prescription (retail) and home delivery) $150 copay per prescription (home delivery) Tier 4 - Typically Specialty (brand and generic) 30% coinsurance up to Not covered (retail and $250 per prescription home delivery) (retail and home delivery) Cost if you use an In- Cost if you use an Covered Vision Benefits Network Provider Out-of-Network Provider This is a brief outline of your vision coverage. To receive the In-Network benefit, you must use a Blue View Vision Provider. Only children's vision services count towards your out-of-pocket limit. Children’s Vision exam (up to age 19) No charge Not covered Limited to 1 exam per benefit period. Page 5 of 9
 Anthem CaliforniaCare HMO Classic 40/60/750 admit/375 OP (TES) Page 4 Page 6
Anthem CaliforniaCare HMO Classic 40/60/750 admit/375 OP (TES) Page 4 Page 6