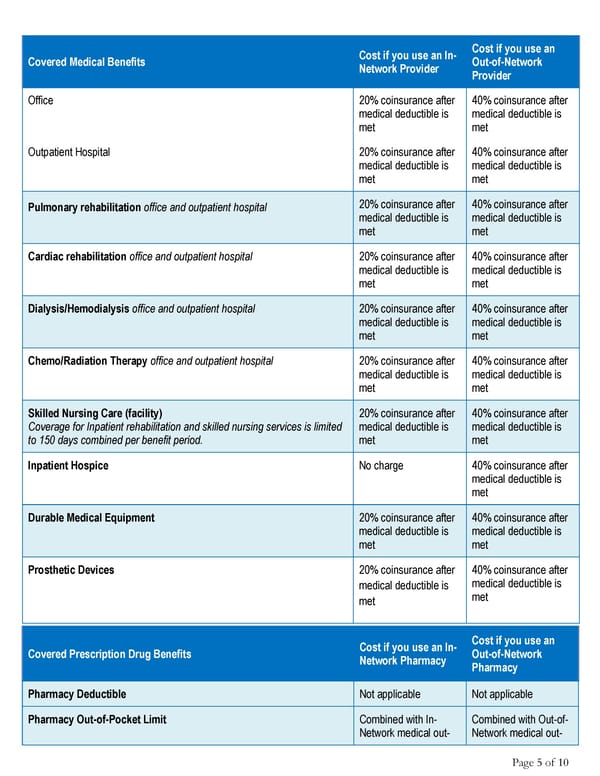
Cost if you use an In- Cost if you use an Covered Medical Benefits Network Provider Out-of-Network Provider Office 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Outpatient Hospital 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Pulmonary rehabilitation office and outpatient hospital 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Cardiac rehabilitation office and outpatient hospital 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Dialysis/Hemodialysis office and outpatient hospital 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Chemo/Radiation Therapy office and outpatient hospital 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Skilled Nursing Care (facility) 20% coinsurance after 40% coinsurance after Coverage for Inpatient rehabilitation and skilled nursing services is limited medical deductible is medical deductible is to 150 days combined per benefit period. met met Inpatient Hospice No charge 40% coinsurance after medical deductible is met Durable Medical Equipment 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Prosthetic Devices 20% coinsurance after 40% coinsurance after medical deductible is medical deductible is met met Cost if you use an In- Cost if you use an Covered Prescription Drug Benefits Network Pharmacy Out-of-Network Pharmacy Pharmacy Deductible Not applicable Not applicable Pharmacy Out-of-Pocket Limit Combined with In- Combined with Out-of- Network medical out- Network medical out- Page 5 of 10
 Anthem Prudent Buyer PPO Classic 1000/35/55/20 (TES) Page 4 Page 6
Anthem Prudent Buyer PPO Classic 1000/35/55/20 (TES) Page 4 Page 6